We continue the interview with Olga Martínez expert at the Catalan Arthroplasty Register (RACat) and Xaxier Mora, specialist in traumatology and orthopaedic surgery with a Master in biomaterials.
The aim of today’s post is to know a little more about prostheses and the biomaterials used in arthroplasties.
With this post and the previous one, we have wanted to present the opinions of these two professionals.
Are all prostheses the same?
Xavier: No, because each patient is different. Therefore, the orthopaedic surgeon will recommend one type of prosthesis or another, depending on the extent to which the bone is affected, the patients’ age, associated diseases and the daily activity of a the patient.
Olga: At present, there are different types of prosthesis on the market in terms of design, materials used in their manufacture and the way they are anchored to the bone. There are prostheses that range from replacing only a part of the joint to more complex joint replacements in situations where bone damage is extensive.
As a user of the health system, to which hospital should I go to receive the best prosthesis?
Xavier: One cannot talk about better or worse prostheses because all prostheses used for implants have to follow a standardised procedure according to specific international standards, such as those of the American FDA and the European CE seal of approval, for materials that will be implanted in humans. In the same way, hospitals in Catalonia are certified to be able to carry out this type of surgery.
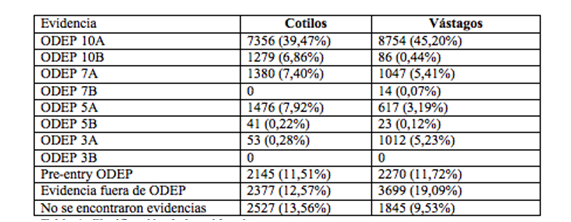
Olga: The prostheses which are commercialised in Catalonia meet the international standards of quality and public hospitals base their choices of prostheses on the scientific evidence available. This is allows them to select those with the best results according to arthroplasty registries, using recommendations from different institutions such as the NICE (National Institute of Healthcare and Clinical Excellence) and the ODEP (Orthopaedic Data Evaluation Panel).
Olga: In addition, the new European legislation passed in 2016, regarding implants used in health, aims to increase the supervision of the industry by implementing stricter norms and regulations including the obligation of clinical assessment, while at the same time fostering innovation in this field.
Who does the research into the best materials available and what factors are taken into account?
Olga: These days, the research of new materials and manufacturing techniques as well as the design and improvement of new prosthetic implants is a multidisciplinary process. The contributions of orthopaedic surgeons are especially important together with studies in joint biomechanics and surgical technique. In Catalonia there are research centres in biomaterials such as Leitat and the Technical University of Catalonia (UPC).
Olga: From the AQuAS we have written up and published short reports on biomaterials (polyethylene, cements and ceramics and metals) aimed at professionals that work in services of orthopaedic surgery and traumatology, with the aim of updating their knowledge.
Reports available in Catalan:
Xavier: Nowadays, when manufacturing new materials, the interaction between the surface of a biomaterial and the bone is taken into account more and more often, so that bone cells can consider an implant as part of its own structure and thereby avoid the prosthesis from moving about because this is one of the biggest problems in getting an implant to function well.
How have materials evolved since the first prostheses to the present day?
Olga: The discovery of new materials and/or the progress made both in terms of manufacturing techniques and the knowledge gained in the biomechanics of the human body have influenced the design of prostheses over time.
Xavier: The first experiences in joint implants date back to the 20s of last century. One of the first attempts at replacing the surface of the head of the hip was done by manufacturing a metal socket or dome (Smith-Petersen).
Xavier: In the last 20 years, many important advances have been made regarding the use of new biomaterials, much safer and of greater resistance to wear, thus extending the life of an implant in a biological environment such as the human body. Together with metallic biomaterials, these days ceramic biomaterials are used with good results in relation to their integration in bone tissue.
Xavier: On the other hand, research in 3D technology has paved the way for a more precise surgery, and in the future it will be possible to manufacture more personalised implants.
Xavier and Olga: We both agree that we are getting closer and closer to having a prosthesis that is for life.